Using social determinants of health to transform employee well-being

The COVID-19 pandemic highlighted stark gaps in communities driven in large part by social determinants of health (SDOH), the aspects of our built environments that can account for up to 80% of differences in health outcomes between individuals.
As employers grapple with the ongoing effects of the pandemic and re-evaluate their corporate wellness programs, SDOH have come to the forefront as an uncompromisable component of effective well-being strategies that put employees first, manage healthcare costs, and position employers as good corporate citizens in their communities.
Over the last year, Sharecare worked with employer-led and public health organizations – the National Alliance of Healthcare Purchaser Coalitions (National Alliance), the National Network of Public Health Institutes, and the Centers for Disease Control and Prevention – to study the role of SDOH in the workplace. With the data and capabilities of the Sharecare Community Well-Being Index, Sharecare analyzed five sub-domains of SDOH across the U.S (illustrated below) to analyze the impact of SDOH on employees and show employers how they could impact health and well-being circumstances that might seem beyond their control. As a result, we identified the social risks in the communities where employees and worksites were located, as well as potential implications for employee well-being, equity, and pandemic recovery goals.
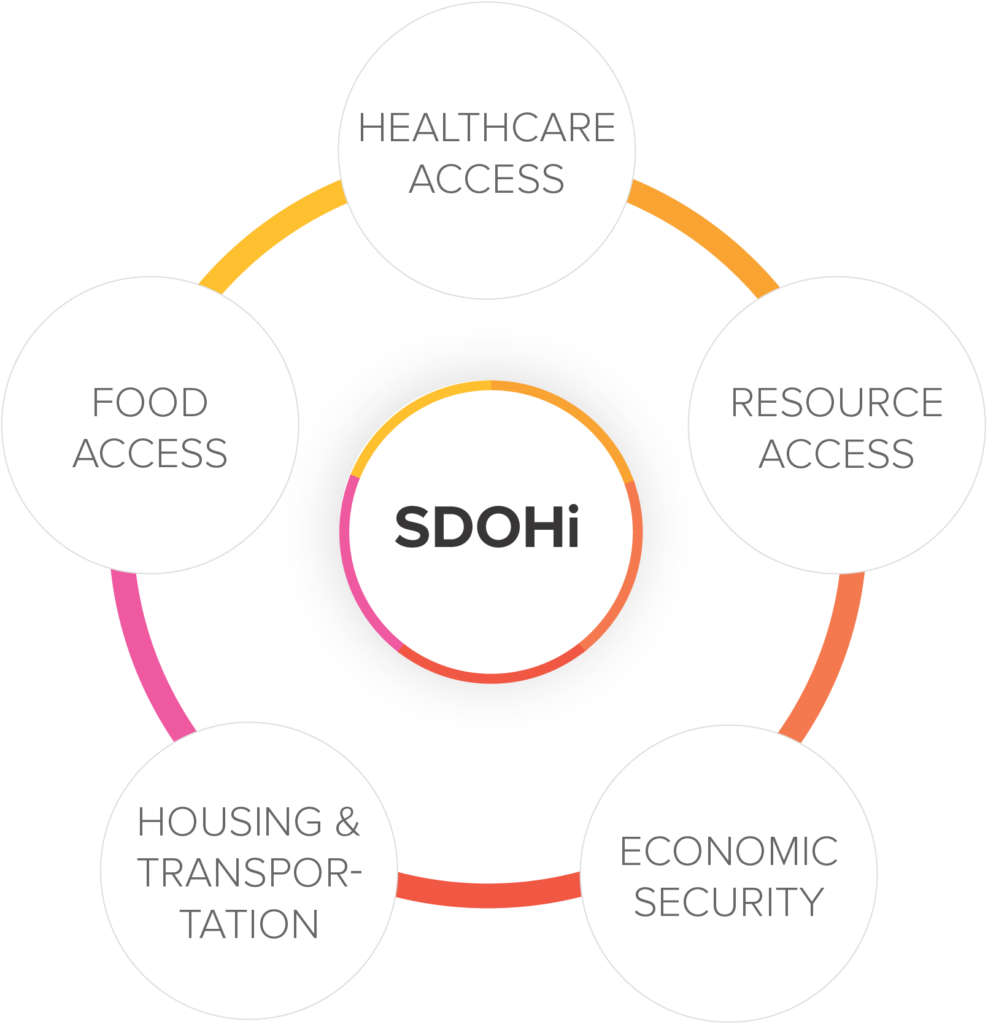
An initial report of findings and lessons learned from six participating employers was published recently by the National Alliance. Among the key takeaways enabled by Sharecare’s Index was an equity trifecta at the nexus of SDOH and potential employer interventions.
The equity trifecta comprises an employee population’s racial and ethnic makeup, salary ranges, and benefits enrollment eligibility and status; and although it does not itself define SDOH, the trifecta offers a way for employers to identify addressable social risk gaps.
At American Eagle Outfitters (AEO), a large American lifestyle, clothing, and accessories retailer, Sharecare’s analysis of the equity trifecta revealed several opportunities to better serve employees at one distribution center in Pennsylvania. Many of these employees reported for in-person work throughout the pandemic, made up part of one of the country’s largest Dominican populations, and lived in a relatively small geographic area. Limited access characterized their community experiences in more ways than one: Not only did gaps in public transportation leave a disconnect between their homes and workplace, but also non-English-speaking households – comprising the majority of AEO’s distribution center employees – had limited access to healthcare resources.
The complete picture painted by the equity trifecta and the SDOH of associates’ communities paved the way for AEO leadership to establish AEO Real Care Health Centers at each of their U.S. distribution centers and ensure the Pennsylvania-based workforce was supported by a bilingual registered nurse. All associates, whether enrolled in AEO’s medical insurance or not, now can access non-acute health services at no cost through the centers; other services, such as virtual visits or acute services, are capped at a $15 copay, significantly minimizing the cost barrier to care. During the study, AEO also began building relationships with local health systems, which sent representatives to discuss vaccines, answer employee questions, and operate free vaccination clinics. To further support associates where they live, AEO introduced English as a Second Language classes in their communities and is partnering with the local transit authority to build new bus stops. Longer-term, AEO is strategizing with internal and external stakeholders to promote health equity among associates and their communities at large.
According to Tammy Fennessy, director of benefits at AEO, the commitment of its associates throughout the COVID-19 pandemic inspired the organization to participate in the study. “We wanted to bring the essential workers in our distribution centers into the conversation because we knew they faced increased risks coming into work every day during the pandemic,” Fennessy said. “We wanted to learn more about them and about how we could help them thrive because they have been a lifeline for us during a difficult time.”
Although the social circumstances of each participating employer’s workforce were different, the study prompted new ways of thinking and led to new well-being strategy imperatives, including taking stock of the needs of employees’ greater communities; recognizing gaps in employee access to healthcare; elevating the roles of data and employee input in strategy-setting; and embracing partnership in the endeavor. In the case of AEO, local health networks and the public transit authority were more than happy to collaborate on efforts to enhance community well-being, demonstrating that employers have ready and willing allies in their midst.
Through our ongoing community well-being research and interventions with employers, Sharecare will continue to share findings and recommendations that account for the full set of risk factors and circumstances that influence employees’ health.